Introduction
Exercise stands as a formidable ally in the fight against type 2 diabetes, paving the way for enhanced insulin sensitivity and improved blood sugar control. Imagine embracing a structured fitness routine that not only boosts your overall health but also lessens your dependence on medication. Yet, the path to effective diabetes management through exercise can feel overwhelming.
How do you navigate the intricate landscape of workout regimens, dietary choices, and your unique health needs? This article explores the best practices for weaving exercise into your diabetes management plan, offering actionable strategies designed to empower you on your journey to wellness.
Understand the Role of Exercise in Type 2 Diabetes Management
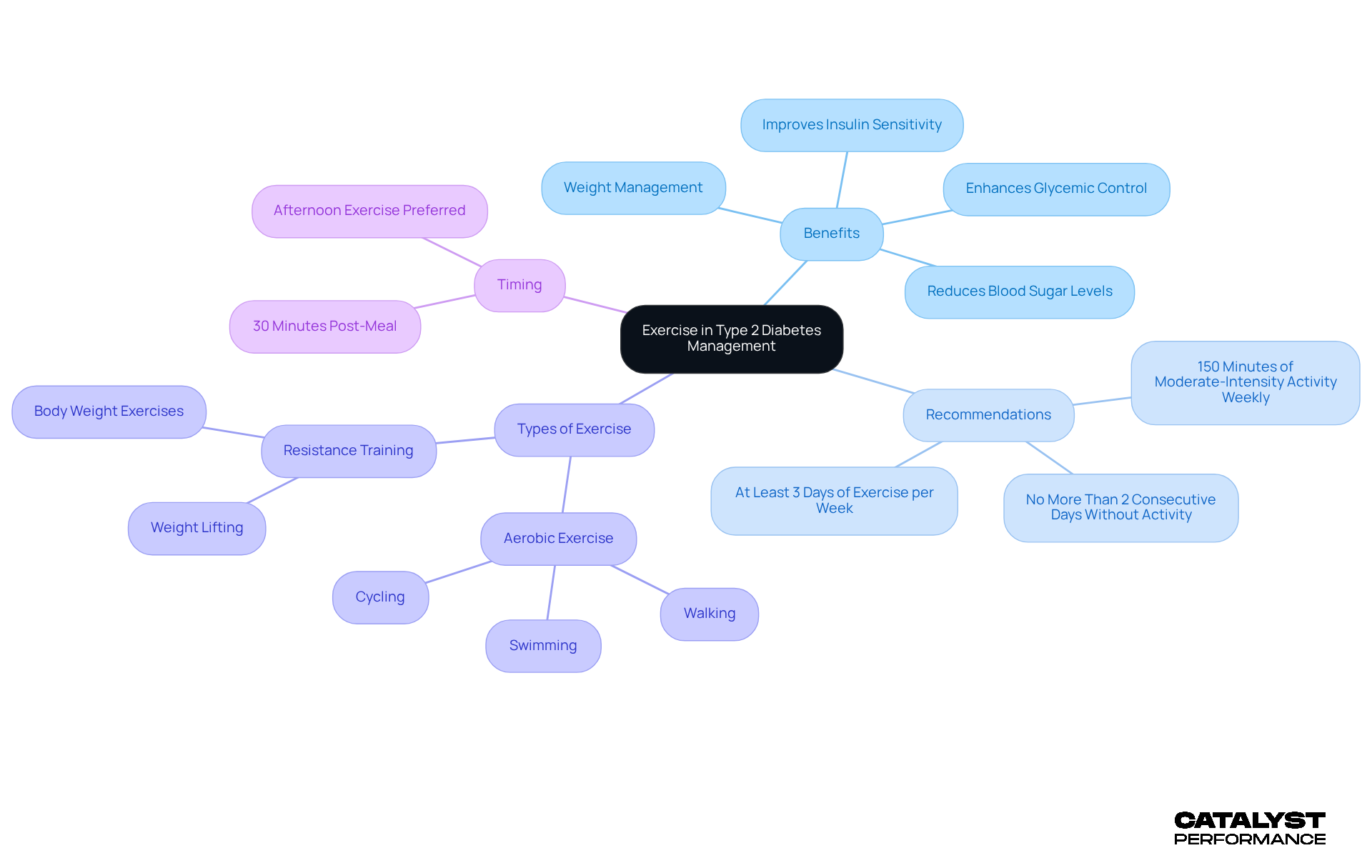
Exercise is a game-changer for those dealing with exercise and type 2 diabetes. It enhances insulin sensitivity, allowing your body to use glucose more effectively. Imagine lowering your blood sugar levels and potentially reducing your need for medication through consistent exercise and type 2 diabetes management. The American Diabetes Association recommends at least 150 minutes of moderate-intensity aerobic activity each week to support exercise and type 2 diabetes management, or 30 minutes of aerobic movement 3 to 7 days a week. This commitment can significantly improve your glycemic control. Plus, exercise and type 2 diabetes management help with weight management, which is crucial since excess weight can worsen insulin resistance.
At [CATALYST PERFORMANCE](https://catalystperformance.sg), we believe in the power of maintaining lean muscle mass - it's a key predictor of longevity and overall health. Incorporating both aerobic and resistance training into your routine can lead to the best results in managing exercise and type 2 diabetes. These two forms of exercise work together to enhance your metabolic health and improve body composition. In fact, regular high-intensity interval training or moderate continuous activity can reverse pre-diabetes in nearly 40% of participants, demonstrating the effectiveness of exercise and type 2 diabetes management! As Steven Malin wisely puts it, 'I think of physical activity as a drug,' emphasizing its vital role in managing exercise and type 2 diabetes.
Timing is also essential; engaging in physical activity about 30 minutes after meals can significantly improve , especially in relation to exercise and type 2 diabetes. This makes your fitness routine not just about what you do, but when you do it. Our CATALYST System is designed to empower individuals of all ages to achieve strength, stability, and health. We want you to enjoy life fully today and for many decades to come.
Implement Effective Exercise Strategies for Diabetes Control
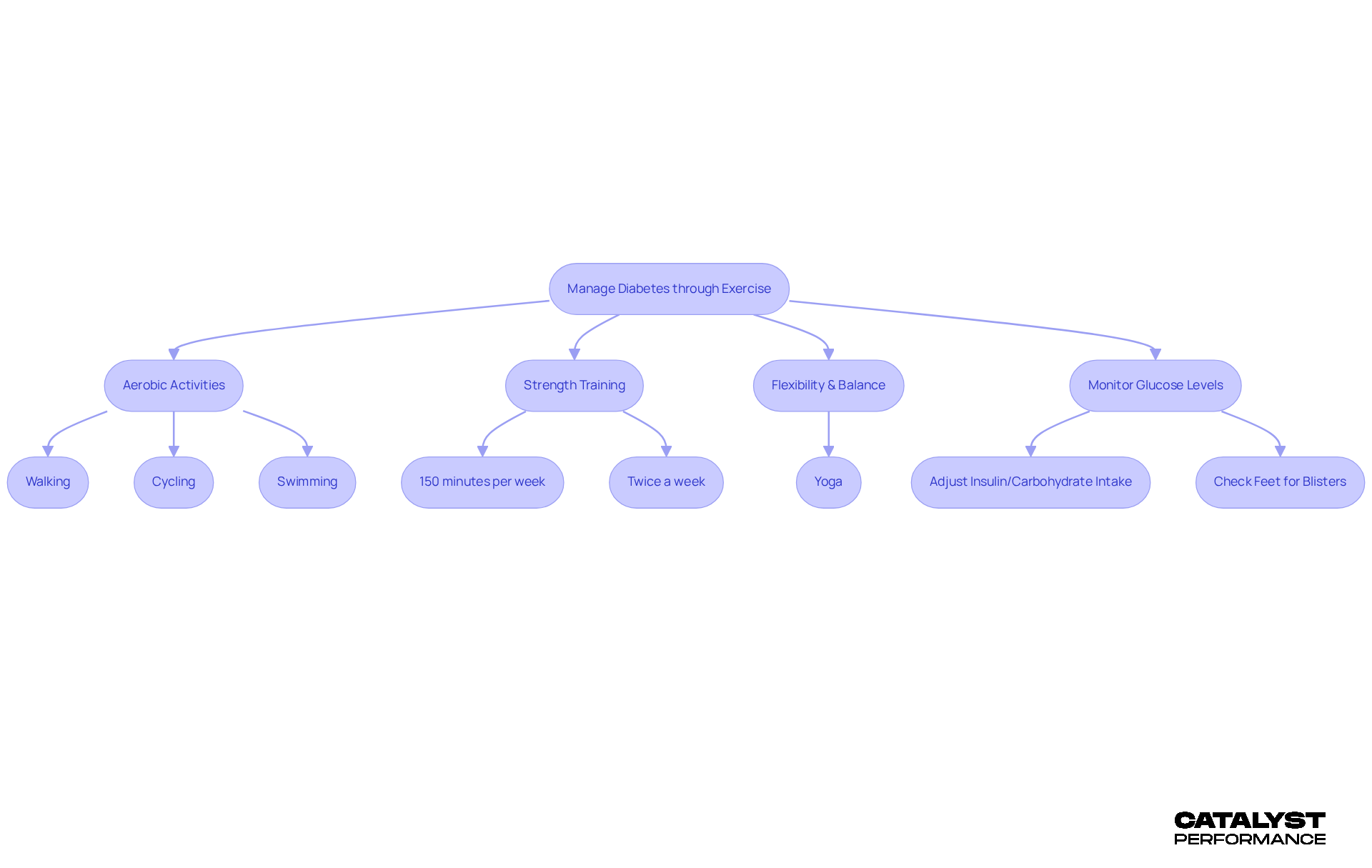
Managing exercise and type 2 diabetes through physical activity can feel daunting, but it’s entirely within your reach. Embracing a balanced routine that includes both aerobic and strength training activities is key. Imagine engaging in activities you enjoy - like walking, cycling, or swimming - for at least 150 minutes each week. Spread this out over several days, and you’re already on your way to better health. Don’t forget about strength training! Aim to incorporate it at least twice a week, focusing on all major muscle groups. This not only enhances your insulin sensitivity but also boosts your overall metabolic health, which is important when considering exercise and type 2 diabetes. And let’s not overlook flexibility and balance activities, such as yoga or tai chi. These practices not only improve your fitness but also lower your risk of injury, making your journey smoother.
Now, let’s talk about the importance of monitoring your glucose readings before and after physical activity. This simple practice can reveal how different activities affect your body, allowing you to make necessary or carbohydrate intake. It’s all about ensuring safe and effective management of your blood sugar levels. And remember, keeping an eye on your feet for blisters before and after exercise is crucial to prevent complications. Consulting with healthcare professionals for personalized fitness recommendations can make a world of difference, especially if you have other medical conditions or complications.
There’s a powerful story here: individuals who commit to these balanced fitness regimens often see remarkable improvements in their A1C readings, which can significantly impact exercise and type 2 diabetes, as well as their overall health. This isn’t just about numbers; it’s about transforming your life. By taking a holistic approach to diabetes management, you can empower yourself to achieve lasting health and wellness. So, take that first step - your journey to better health starts now!
Monitor and Adapt Exercise Plans for Optimal Results
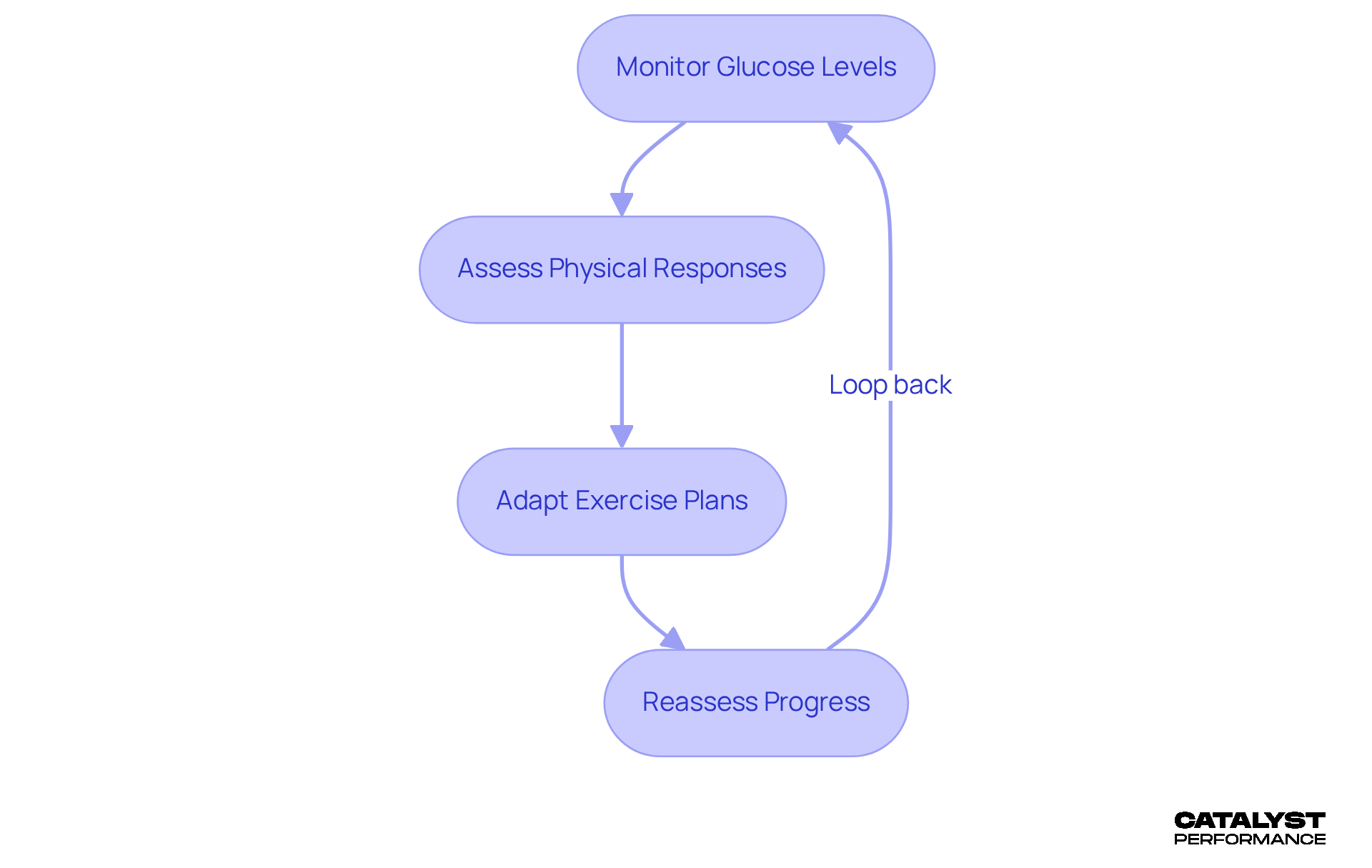
Monitoring your progress is vital if you have Type 2 diabetes and want to maximize your fitness journey through exercise and type 2 diabetes management. Keeping a close eye on your glucose levels before, during, and after workouts isn’t just important; it’s essential. By diligently recording these measurements, you can spot trends that help you make informed adjustments to your activity-whether that means changing the intensity, duration, or frequency of your workouts. If you notice that a specific workout often leads to low glucose levels, it might be time to rethink when or how intensely you’re exercising, or perhaps increase your carbohydrate intake beforehand.
It’s also crucial to tune into how your body feels during and after physical activity. Are you experiencing fatigue or signs of low blood sugar? This [personalized approach to fitness](https://blog.catalystperformance.sg/4-best-practices-for-setting-personal-training-prices-effectively) is supported by the 2026 ADA Standards of Care, which stress the importance of tailored activity plans that cater to your unique needs and glucose levels. Research shows that structured physical activity programs can significantly improve glycemic control, with a recommendation of at least 150 minutes of moderate-to-vigorous activity each week.
Real-life examples reveal that individuals who consistently monitor their glucose levels while exercising are more likely to achieve better health outcomes. This highlights the importance of adapting your workout plans for optimal results. At [CATALYST PERFORMANCE](https://catalystperformance.sg), we assess you at baseline, then reassess at week sixteen, and every twelve to sixteen weeks thereafter, depending on your goals and training frequency. This structured reassessment process allows us to track your progress in body composition, cardiorespiratory fitness, stability, and strength, ensuring your program reflects your current capabilities.
This method is particularly beneficial for those managing exercise and type 2 diabetes, as it helps customize workout plans to meet your evolving needs and enhances your ability to manage glucose levels effectively. Plus, our coaches are here to guide you every step of the way, focusing on movement quality, comfort, and confidence. This support makes it easier for individuals with busy schedules to stay on track. Utilizing (CGMs) can further enhance your ability to track glucose levels, providing valuable insights to inform your activity choices.
Integrate Exercise with Nutrition and Lifestyle for Comprehensive Management
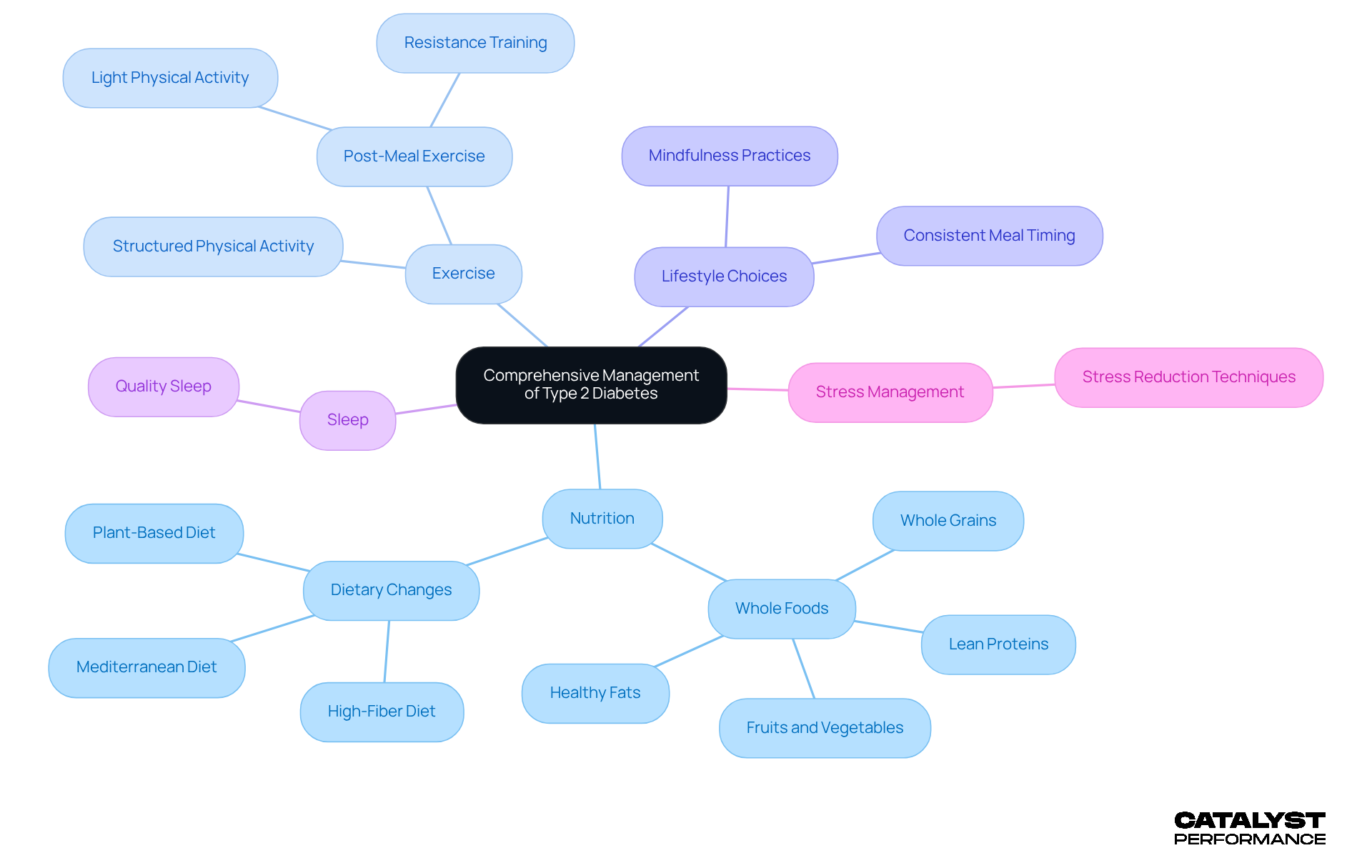
Managing Type 2 diabetes effectively is all about taking charge of your health through a blend of exercise, a balanced diet, and smart lifestyle choices. Imagine a diet filled with whole foods - think vibrant fruits, crisp vegetables, hearty whole grains, lean proteins, and healthy fats. This isn’t just about eating well; it’s about empowering your body to regulate sugar and enhance your overall health. Research shows that making organized dietary changes can lead to impressive improvements in glycemic control, with HbA1c values dropping by as much as 1.8% when you commit to lifestyle adjustments.
But it doesn’t stop there. Meal timing plays a pivotal role too. Exercising after meals can be a game-changer for your blood sugar levels. Picture this: engaging in light physical activity right after eating can significantly lower your post-meal glucose levels, with reductions of up to 85 mg/dL in some cases. This powerful connection between diet and physical activity highlights the importance of a to managing diabetes.
And let’s not forget about the impact of a good night’s sleep and stress management. Incorporating mindfulness practices can boost your insulin sensitivity and overall well-being. Partnering with healthcare professionals - like dietitians and diabetes educators - can provide you with tailored guidance to create a comprehensive plan that harmonizes exercise, nutrition, and lifestyle. This holistic approach not only enhances blood sugar control but also nurtures your long-term health and vitality.
However, it’s crucial to stay vigilant about common pitfalls. Neglecting meal timing or losing consistency in your dietary choices can slow your progress. Remember, every step you take towards managing your diabetes is a step towards a healthier, more vibrant you. Embrace the journey, and believe in your ability to achieve lasting health and fitness!
Conclusion
Embracing an active lifestyle is essential for taking charge of Type 2 diabetes. Regular exercise not only boosts insulin sensitivity but also plays a crucial role in managing blood sugar levels, maintaining a healthy weight, and enhancing overall well-being. By weaving physical activity into daily routines, individuals can significantly lessen their dependence on medication and elevate their quality of life.
This article shines a light on effective strategies for exercise management in the realm of Type 2 diabetes. It emphasizes the importance of:
- Committing to at least 150 minutes of moderate-intensity aerobic activity each week
- Incorporating strength training
- Timing workouts wisely to optimize glucose regulation
Keeping an eye on glucose levels before, during, and after exercise is vital; it allows for personalized adjustments that can lead to better health outcomes. Moreover, pairing exercise with a balanced diet and healthy lifestyle choices amplifies the positive effects on blood sugar control.
Ultimately, the journey to managing Type 2 diabetes through exercise is a holistic one. It calls for a commitment not just to physical activity but also to nutrition, sleep, and stress management. By taking proactive steps and seeking guidance from healthcare professionals, individuals can empower themselves to achieve lasting health and vitality. The path may be challenging, but with determination and the right strategies, a healthier future is absolutely within reach.
Frequently Asked Questions
How does exercise impact type 2 diabetes management?
Exercise enhances insulin sensitivity, allowing the body to use glucose more effectively, which can lower blood sugar levels and potentially reduce the need for medication.
What is the recommended amount of exercise for managing type 2 diabetes?
The American Diabetes Association recommends at least 150 minutes of moderate-intensity aerobic activity each week, or 30 minutes of aerobic movement 3 to 7 days a week.
Why is weight management important for individuals with type 2 diabetes?
Weight management is crucial because excess weight can worsen insulin resistance, making diabetes management more challenging.
What types of exercise are beneficial for managing type 2 diabetes?
Both aerobic and resistance training are beneficial. Incorporating these two forms of exercise can enhance metabolic health and improve body composition.
Can exercise reverse pre-diabetes?
Yes, regular high-intensity interval training or moderate continuous activity can reverse pre-diabetes in nearly 40% of participants.
When is the best time to engage in physical activity for glucose regulation?
Engaging in physical activity about 30 minutes after meals can significantly improve glucose regulation.
What is the CATALYST System?
The CATALYST System is designed to empower individuals of all ages to achieve strength, stability, and health, promoting an active lifestyle for long-term well-being.




